|
Introduction Pilates is a versatile and accessible form of exercise that has gained popularity for its numerous health benefits. Whether you are an athlete, a senior, or someone recovering from an injury, Pilates can be tailored to meet your needs. One of the most significant advantages of Pilates is its ability to alleviate low back pain, a common ailment affecting millions worldwide. In this blog, we'll explore why Pilates is a form of exercise everyone can and should do, and how it can help heal low back pain. What is Pilates? Pilates is a low-impact exercise regimen developed by Joseph Pilates in the early 20th century. It focuses on core strength, flexibility, and overall body awareness through controlled, precise movements. The exercises can be performed on a mat or using specialized equipment such as the Reformer, Cadillac, and Wunda Chair. Why Pilates is for Everyone 1. Adaptable for All Fitness Levels: Pilates exercises can be modified to suit beginners and advanced practitioners alike. This makes it an excellent choice for people of all ages and fitness levels. 2. Low-Impact: The gentle nature of Pilates reduces the risk of injury, making it suitable for those with joint issues or recovering from surgery. 3. Holistic Approach: Pilates focuses on the mind-body connection, promoting mental well-being alongside physical health. 4. Improves Posture: Poor posture is a common issue that can lead to various health problems. Pilates emphasizes proper alignment and strengthens the muscles responsible for maintaining good posture. 5. Enhances Flexibility: Regular practice increases flexibility, reducing the risk of muscle strains and improving overall mobility. 6. Core Strengthening: A strong core is essential for overall stability and balance, and Pilates is renowned for its ability to build core strength effectively. How Pilates Helps Heal Low Back Pain Low back pain is a pervasive issue that can stem from various causes such as poor posture, muscle imbalances, and a sedentary lifestyle. Pilates addresses these underlying issues through targeted exercises that strengthen, stretch, and stabilize the muscles supporting the spine. 1. Core Strengthening: The core muscles, including the abdominals, obliques, and lower back muscles, play a crucial role in supporting the spine. Pilates exercises such as the "Hundred" and "Plank" strengthen these muscles, providing better support for the lower back. 2. Improved Posture: Poor posture can lead to low back pain by placing undue stress on the spine. Pilates emphasizes alignment and awareness, helping to correct postural imbalances and reduce strain on the lower back. 3. Increased Flexibility: Tight muscles, particularly in the hips and hamstrings, can contribute to low back pain. Pilates incorporates stretching exercises that increase flexibility, alleviating tension and improving range of motion. 4. Balanced Muscle Development: Imbalances between muscle groups can lead to pain and injury. Pilates promotes balanced muscle development, ensuring that no single muscle group is overworked or neglected. 5. Enhanced Body Awareness: Pilates fosters a heightened sense of body awareness, helping individuals recognize and correct movement patterns that may contribute to low back pain. Key Pilates Exercises for Low Back Pain 1. Pelvic Clock 2. 90/90 Abdominal Marching 3. Bridging 4. Cat/Cow 5. Pointer Dog Access & subscribe to our YouTube below for more exercises to condition your core and improve your quality of life & health! Tips for Practicing Pilates Safely
1. Consult a Professional: Before starting a Pilates routine, consult with a healthcare provider or a certified Pilates instructor, especially if you have a history of low back pain. 2. Start Slow: Begin with basic exercises and gradually progress to more advanced movements as your strength and flexibility improve. 3. Listen to Your Body: Pay attention to your body’s signals. If an exercise causes pain, stop immediately and seek guidance from your instructor. 4. Maintain Consistency: Regular practice is key to seeing improvements. Aim for consistent, moderate sessions rather than sporadic intense workouts. Conclusion Pilates is a form of exercise that truly everyone can benefit from. Its adaptable nature, focus on core strength, and holistic approach make it suitable for individuals of all ages and fitness levels. For those suffering from low back pain, Pilates offers a safe and effective way to strengthen the core, improve posture, and enhance flexibility, leading to lasting relief and improved quality of life. Embrace Pilates as a part of your fitness routine and experience the transformative benefits it has to offer.
0 Comments
Understanding the Core The term "core" is often mentioned in fitness circles, but what exactly does it mean? The core is more than just a buzzword; it is the powerhouse of your body, crucial for stability, balance, and overall health. Conditioning your core through exercises like Pilates can significantly decrease spinal pain and enhance your overall quality of life. In this blog, we'll delve into what the core is, its importance, and how Pilates can be a transformative practice for spinal health and well-being. What is the Core? The core encompasses a group of muscles located in the abdomen, lower back, hips, and pelvis. These muscles work together to support the spine, maintain posture, and facilitate movement. Key muscles in the core include: 1. Rectus Abdominis: Often referred to as the "six-pack" muscles, these run vertically along the front of the abdomen. 2. Transverse Abdominis: Located deep within the abdomen, this muscle stabilizes the spine and pelvis. 3. Internal and External Obliques: These muscles are on the sides of the abdomen and assist in twisting and bending movements. 4. Erector Spinae: A group of muscles along the spine that help maintain an upright posture. 5. Multifidus: Deep muscles along the spine that provide stability and support. 6. Pelvic Floor Muscles: These muscles support the pelvic organs and contribute to core stability. 7. Diaphragm: The primary muscle used in breathing, which also plays a role in core stability. Why is Core Conditioning Important? 1. Spinal Stability: A strong core supports the spine, reducing the risk of injuries and alleviating chronic pain. 2. Improved Posture: Core muscles help maintain proper posture, which is essential for reducing strain on the spine and preventing musculoskeletal issues. 3. Enhanced Balance and Coordination: A stable core is crucial for balance and coordination, reducing the risk of falls and improving overall movement efficiency. 4. Better Performance in Daily Activities: Whether lifting, bending, or twisting, a strong core makes everyday tasks easier and safer. 5. Injury Prevention: Conditioning the core can prevent injuries, particularly in the lower back, by ensuring that the spine is properly supported during movement. How Pilates Conditions the Core Pilates is renowned for its emphasis on core strength and stability. Here’s how Pilates can condition the core and lead to significant health benefits: 1. Targeted Exercises: Pilates focuses on precise movements that engage and strengthen the core muscles. Exercises such as the "Hundred," "Plank," and "Roll-Up" are designed to challenge the core and build endurance. 2. Controlled Movements: Pilates emphasizes slow, controlled movements that enhance muscle activation and promote stability. This approach reduces the risk of injury and ensures that the core muscles are effectively engaged. 3. Breath Control: Proper breathing techniques are integral to Pilates. Coordinating breath with movement enhances core engagement and supports spinal stability. 4. Flexibility and Strength: Pilates combines strength training with stretching, ensuring that the core muscles are not only strong but also flexible. This balance is crucial for preventing muscle imbalances and maintaining optimal spinal health. 5. Mind-Body Connection: Pilates encourages a strong mind-body connection, promoting awareness of how the body moves and ensuring that core muscles are activated during daily activities. Key Pilates Exercises for Core Conditioning 1. Abdominal Marching 2. Abdominal Toe Taps 3. Core Stabilization on the Foam Roll 4. Pointer Dog Access & subscribe to our YouTube below for more exercises to condition your core and improve your quality of life & health! Conclusion Understanding and conditioning the core is essential for spinal health and overall well-being. Pilates offers a comprehensive approach to strengthening the core, reducing spinal pain, and improving quality of life. By incorporating Pilates into your fitness routine, you can achieve a stronger, more stable core, better posture, and enhanced mobility, leading to a healthier, more vibrant life. Many of us understand that we should be getting more sleep for greater health benefits , but may not appreciate exactly why and how. A few reasons why good, restful sleep is so important... : 1. Weight Maintenance or Loss Numerous studies have associated short sleep, (defined as sleeping fewer than 7 hours per night), with a greater risk of weight gain. The effect of sleep on weight gain is believed to be affected by a few reason including hormones and motivation to exercise. Ghrelin is a hormone that makes us feel hungry while leptin makes us feel full. Sleep deprivation increases levels of ghrelin and decreases levels of leptin. This may cause us to feel hungrier and overeat. This is supported by various studies that have shown that sleep-deprived individuals have a bigger appetite and tend to eat more calories. 2. Heart Health Low sleep quality and duration may increase your risk of developing heart disease. An analysis of 19 studies found that sleeping fewer than 7 hours per day resulted in a 13% increased risk of death from heart disease. Short sleep also appears to increase the risk of high blood pressure. In fact, one study found that people who slept fewer than 5 hours per night had a 61% higher risk of developing high blood pressure than those who slept for 7 hours. 3. Immune system strength During sleep, your body releases cytokines, which are essential for the regulation of the immune system. Cytokines are required in increased amounts when you are attacked by a pathogen or are under stress. The level of cytokines increase during sleep, and therefore lack of sleep hinders the body's ability to fight infections. This is also a reason why the body tends to sleep more while suffering from any infection. 4. Mental Health Mental health concerns, such as depression, are strongly linked to poor sleep quality and sleeping disorders. One study in 2,672 participants found that those with anxiety and depression were more likely to report poorer sleep scores than those without anxiety and depression. In other studies, people with sleeping disorders i.e. insomnia or destructive sleep apnea were noted to have a statistically significant correlation to poor mental health status. 5.Healing Properties & Inflammation Management Lastly, but almost most importantly for Pilates Sante clients, poor sleep is linked to increased inflammation in the body. Sleep loss, especially from disturbed sleep, is known to activate inflammatory signaling pathways and lead to higher levels of undesirable markers of inflammation, like interleukin-6 and C-reactive protein limiting healing of injury or pathology in the body. So what are some ways we can try to improve our sleep quality ? 1. Increase Bright Light Exposure During the Day
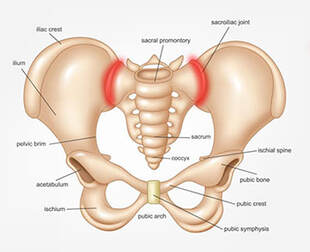
Your body has a natural time-keeping clock known as your circadian rhythm. It affects your brain, body, and hormones, helping you stay awake and telling your body when it is time to sleep. Natural sunlight or bright light during the day helps keep a healthy circadian rhythm. This improves daytime energy, as well as nighttime sleep quality and duration. 2. Reduce Blue Light Exposure in the Evenings Blue light -- which electronic devices like smartphones and computers emit in large amounts —tricks your brain into thinking it’s still daytime. This reduces hormones such as melatonin, which help you relax and get deep sleep. There are several popular methods you can use to reduce night blue light exposure such as wearing glasses that block blue light & limiting use for phones, computers, and TV at least 2 hrs before bed. 3. Do not Consume Caffeine at Later Periods in the Day Caffeine stimulates your nervous system and may stop your body from naturally relaxing at night. It can stay elevated in your blood for 6 to 8 hours! Therefore, drinking coffee or other caffeinated beverages after 3 to 4 p.m. is not recommended, especially if you are sensitive to caffeine or have trouble sleeping. 4. Limit Alcohol Consumption Having a couple of drinks at night can negatively affect your sleep and hormones. It alters nighttime melatonin production, which plays a key role in your body’s circadian rhythm. Alcohol is known to cause or increase the symptoms of sleep apnea, snoring, and disrupted sleep patterns. 5. Try to Sleep & Wake at Consistent Times Your body’s circadian rhythm functions on a set loop, aligning itself with sunrise and sunset. Irregular sleep patterns can alter your circadian rhythm and levels of melatonin, which signal your brain to sleep. Being consistent with your sleep & waking times can aid long-term sleep quality. 6. Consider Sleep-Supporting Supplements i.e.: - Melatonin - CBD - Ginkgo biloba - Glycine - Valerian root - Magnesium - L-theanine If none of the above measures are helping your sleep hygiene, please consider seeing a healthcare provider for a sleep evaluation. There are many common conditions that can cause poor sleep, including sleep apnea. Many of our clients that come to Pilates Santé have pain due to excessive inflammation. The inflammatory response is a normal process of recovering from injury. However, when the inflammation becomes excessive, it slows the natural healing our bodies. A lot of our clients are attempting to wean off medications, and working with your diet is a very effective method of doing so. We now have the research to prove there are very effective ways to significantly reduce inflammation through diet. Common foods to eliminate that cause inflammation: • Refined carbohydrates such as white bread & sugar • French fries & other foods • Soda & other sweetened beverages • Processed meat such as hot dogs & sausages • Excessive alcohol Foods to add that manage or help decrease the inflammatory process: • Berries • Fatty fish i.e.: salmon, tuna & sardines • Green, leafy vegetables • Avocados • Mushrooms • Green tea • Turmeric • Bone broth • Olive oil • Nuts i.e.: almonds & walnuts These healthy foods cannot only help with musculoskeletal injury & pain, however can also prevent systemic disease of all kinds including: • Diabetes • Cancer • Heart disease If you’re looking for a specific anti-inflammatory diet prescribed for your needs and restrictions, we highly recommend seasoned nutritionist Tammy Parkinson. Nutritionally, Tammy works on a variety of health complexities ranging from inflammatory issues, to auto immune disorders, to metabolic and blood work complications to basic lifestyle, weight management and wellbeing modifications. Learn more about Tammy’s work and experience at her website here: https://www.mybodyfirm.com/ 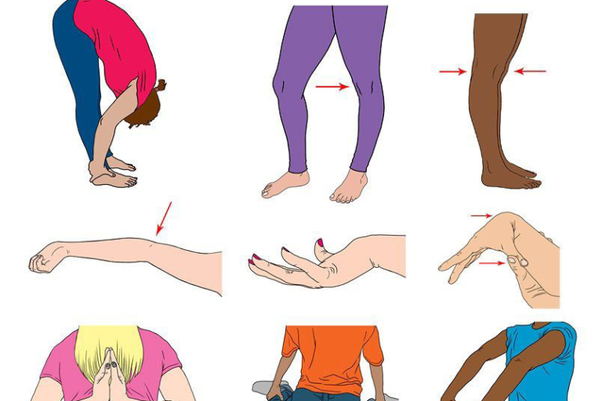 Hypermobility Syndrome (HMS) is not completely understood yet, but is grossly defined as a connective tissue abnormality which causes excessive mobility of joint or soft tissues of the musculoskeletal system. It also impacts cardiac tissue, smooth muscle of the genital system, and the gastrointestinal system. Often HMS is misdiagnosed or overlooked because of the myriad of symptoms that can present with it. Common complaints & injuries for HMS patients include, but are not limited to:
Common conditions that can cause hypermobility:
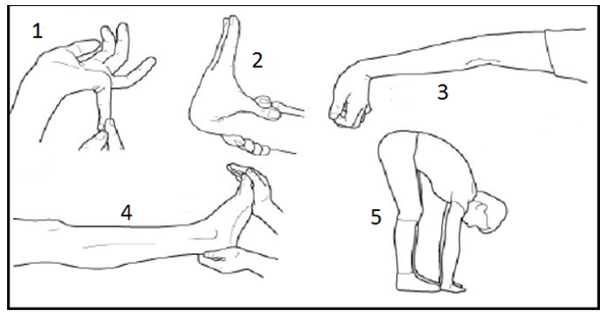
How is HMS currently diagnosed by physicians & other health practitioners? Often by use of the Beighton test or score Beighton Score of ≥ 4/9 & Arthralgia (joint pain) for > 3 months in > 4 joints. The Beighton Test: 1. A passive dorsiflexion of the little finger above 90 degrees, (1 point for each hand). 2. Bringing the thumb passive against the ventral side of the forearm, (1 point for each thumb). 3. Hyperextension of the elbow above 10 degrees, ( 1 point for each elbow). 4. Hyperextension of the knee above 10 degrees, (1 point for each knee). 5. Flexion of the trunk, whit knees straight & palms flat on the ground, (1 point). Other diagnostic factors can include:
Treatment often consists of pain management & therapeutic exercises which include: proprioceptive & motor control, stabilization & strengthening of affected joints & tissues. So... How can Pilates exercises help? The Pilates method of exercise is based on quality of movement, control and body awareness teaching clients with HMS how to move more safely. Exercises on equipment such as the reformer & cadillac can use resistance springs in an anti-gravity position to safely stabilize & strengthen the hypermobile areas of these clients. At Pilates Sante, a large majority of our clients have HMS, (often not medically diagnosed), who benefit greatly from a regular and safe Pilates-based home exercise program, in addition to private sessions administered by a physical therapist or highly trained pilates instructor. For more information about HMS, see resources below.
Resources: *https://www.physio-pedia.com/Hypermobility_Syndrome *https://www.hypermobility.org/types-of-hms  There are a variety of problems and pathology that cause low back pain. These range from joint inflammation, soft tissue and facial tightness, disc herniation, degenerative disc disease, stenosis and lumbar nerve root inflammation or impingement. Low back pain is second only to the common cold as a reason for doctor office visits in the United States. Why is low back pain so common? Today’s jobs and functional activities are contributing to worsening posture and body mechanics, causing increased load and stress to the spine. One common pathology we see here (but it doesn't account for all of our back pain patients) is Degenerative Disc Disease, or DDD. It is the process of losing disc height. The inner most part of the intervertebral disc, called the nucleus pulposus, loses fluid and often small cracks or fissures develop in outer annulus of disc. DDD is not necessarily a "normal" process of aging, but a common process. It is often a progression of previous disc herniation or bulge, but can occur at the same time. DDD can occur in individuals as young as 30 years old, and into 90 years of age. Common Symptoms of DDD include :
How do we treat back pain?All current research concludes that the only long-term effective treatment for low back pain of all pathologies is therapeutic exercise. Other modalities, such as massage, joint mobilization, or electrical stimulation are not strongly supported by research at this time. So what is therapeutic exercise? It is exercise which helps to facilitate support and healing of the injured tissue. The specific exercises prescribed must be related to the type of pathology or structure creating the low back pain. Pilates has become one of the most commonly prescribed therapeutic exercise treatments for low back pain. The movement principles of Pilates align with what allows for the extremely efficient healing of low back pain. The Principles of Pilates:
Our clients feel the benefits early on in their program, and most often continue working with us even after symptoms have resolved. Our physical therapists and pilates instructors work together to continue tailoring your exercise program. We grow alongside you at every step of your journey. Our primary goal is to allow our clients to heal and return to a fulfilling, pain-free lifestyle. Below is a brief video of intermediate level core exercises generally safe for most low back conditions. However we strongly encourage you to meet with us for an individual evaluation, so exercises can be tailored specifically to your spine condition. What is Osteopenia & Osteoporosis?Osteopenia is a condition where bone mineral density is lower than normal. Its defined as a bone mineral density score between -1.0 and -2.5, and is considered by many doctors to be a precursor to osteoporosis. Osteoporosis is a progressive bone disease that is characterized by a decrease in bone mass and density which can lead to an increased risk of fracture. Osteoporosis is defined as a bone mineral density score of -2.5 standard deviations or more below the mean peak bone mass. Medication is typically indicated. What are the risk factors for these conditions?
What are the complications of these conditions?Bone fractures, particularly in the spine or hip, are the most serious complication of osteoporosis. Hip fractures often are caused by a fall and can result in disability and even an increased risk of death within the first year after the injury. In some cases, spinal fractures can occur even if you haven't fallen causing back pain, lost height and a hunched forward posture. How is Osteopenia & Osteoporosis treated?Treatment varies considerably among physicians and practitioners, but usually includes hormone balancing, exercises specific for bone health, a healthy diet rich in calcium, vitamin D and magnesium, and bone building supplements or medications. Exercises which improve posture (decreasing round back kyphosis position), strengthen the spinal muscles and hip muscles in particular. Balance exercises are also important to decrease fall risk, and potential fracture related to falls. Below you can find: |
Ariel Lehaitre, AuthorCategories |
Proudly powered by Weebly